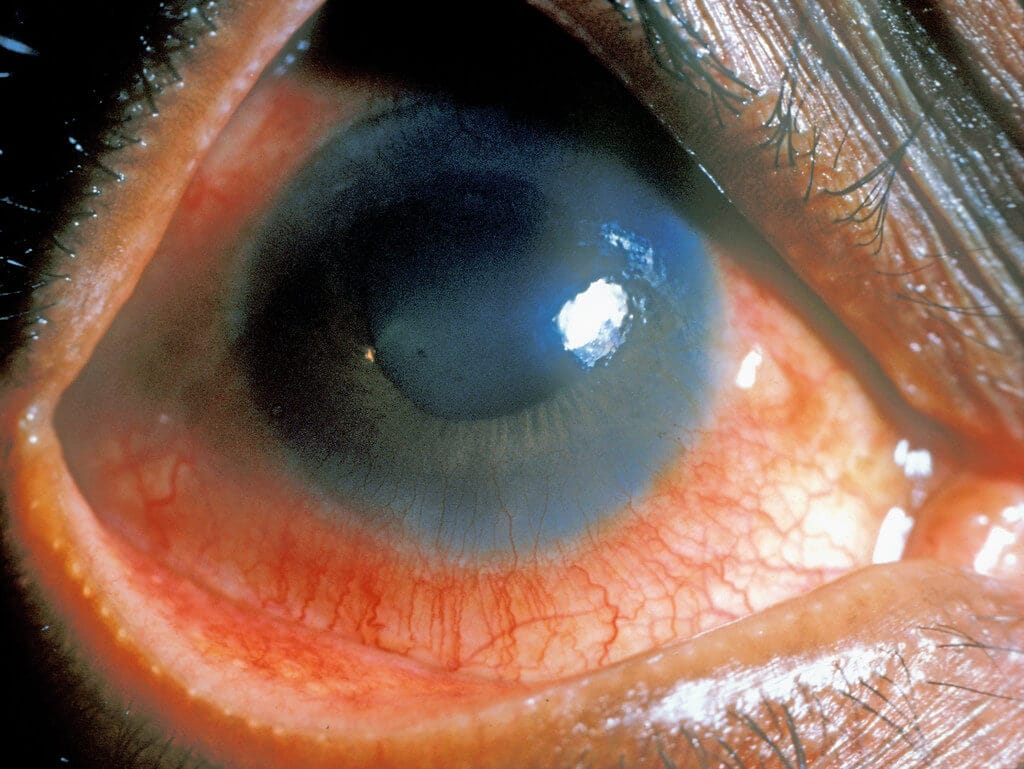
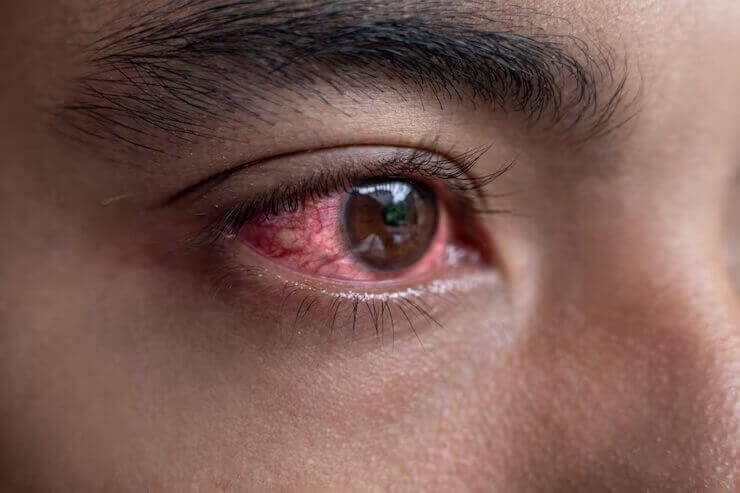
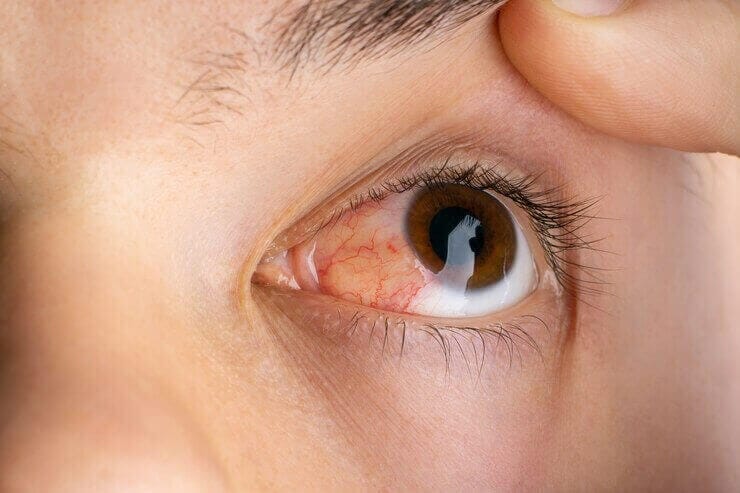
Treatment Options for Uveitis
Understanding your treatment options for uveitis in greater detail can help you make informed decisions about your eye health. Here's an in-depth look:
Eye Drops
Corticosteroids: Predominantly used for anterior uveitis, these drops help control inflammation directly at the eye's surface. A study published in the Ophthalmology journal found that topical corticosteroids like prednisolone acetate were effective in treating anterior uveitis, achieving control of inflammation in up to 90% of cases. However, it's essential to consider side effects and long-term risks associated with each treatment option. Corticosteroids can cause increased intraocular pressure, glaucoma, and cataract formation when used long-term.
Antibiotic Eye Drops: If an infection is present, these may be used alongside steroid drops.
Cycloplegic Drops: These dilate the pupil and prevent muscle spasms, offering pain relief.
Oral Steroids
Prednisone: The most commonly prescribed oral steroid, it works by suppressing the entire immune response, not just in the eyes.
Duration and Side Effects: Usually a short-term treatment due to potential side effects like weight gain, osteoporosis, and increased blood sugar.
Immune-Modulating Medications
Methotrexate and Azathioprine: These medications are usually taken orally and can control inflammation by modulating the immune system.
Biologics: Biologic therapies, such as adalimumab (Humira), have also shown promise. The VISUAL I and VISUAL II clinical trials found that patients treated with adalimumab had a significantly lower risk of uveitis flare or visual impairment compared to those on placebo.
Anti-Inflammatory Drugs
NSAIDs: Available both in oral form and as eye drops, they can offer additional inflammation and pain control but are usually less potent than steroids.
Antiviral or Antibiotic Medications
Valacyclovir or Acyclovir: These antiviral medications are used for uveitis caused by herpes viruses.
Doxycycline: This antibiotic may be used for Lyme disease-associated uveitis.
Injectable Treatments
Intravitreal Injections: Medications like triamcinolone can be injected directly into the eye for intermediate and posterior uveitis.
Steroid Implants: Slow-release devices can provide medication over a longer period, minimizing the need for frequent injections.
Surgery
Vitrectomy: Removal of the vitreous gel to reduce inflammation. Usually reserved for severe cases that do not respond to other treatments.
Scleral Buckle: Rarely used, this procedure can help reattach a detached retina caused by uveitis.
Monitoring and Follow-up
Regular Exams: Patients need to be closely monitored with frequent eye examinations to assess treatment effectiveness.
Treatment Adjustments: Based on the exams, medication types or dosages may be adjusted.
Lifestyle Changes
Smoking Cessation: Smoking can worsen uveitis and reduce treatment effectiveness.
Stress Management: Stress can trigger autoimmune responses, so techniques like meditation may be beneficial.
Does Uveitis Affect Both Eyes?
The question of whether uveitis affects one or both eyes can be crucial for diagnosis and treatment. Here's what you need to know:
Usually One Eye, But Not Always
Most commonly, uveitis initially presents in one eye. Anterior uveitis, the most common type, usually affects just one eye. However, it's possible for the other eye to become involved over time.
Bilateral Cases
In some instances, especially with intermediate and posterior uveitis, both eyes may be affected. This is more likely when the uveitis is related to systemic conditions like lupus or rheumatoid arthritis.
Severity May Vary
If both eyes are affected, the severity might not be the same in both. One eye could have mild symptoms, while the other could be more severely affected.