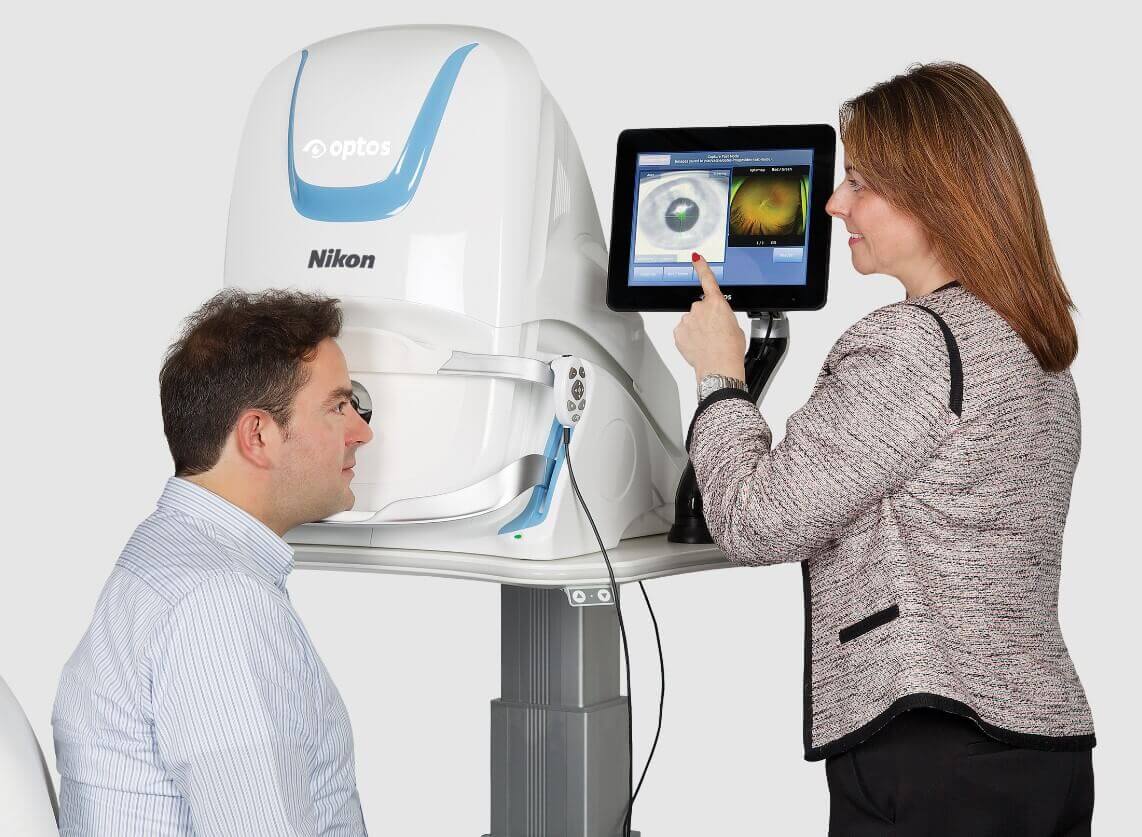
Do I need to go to an emergency room or eye doctor for an eye infection?
It is always advisable to schedule an emergency eye exam with either an optometrist or ophthalmologist if you have an eye infection. In certain situations where the only available care is urgent care or an emergency room, you may be advised to go there, however in general eye doctors have the equipment and training to best diagnose and treat eye infections of all types.
While each situation is different, we have listed some potentially serious symptoms that require immediate medical attention. This list is not a replacement for an eye doctor, and if you are unsure it is always advisable to call an eye doctor to get specific guidance.
Symptoms that require an emergency eye exam
These symptoms suggest a potentially serious condition that requires immediate evaluation by an eye doctor:
Severe eye pain: Intense and persistent eye pain that is not relieved with over-the-counter pain relievers should be evaluated promptly.
Sudden vision changes: Any sudden loss of vision, whether partial or complete, warrants immediate attention.
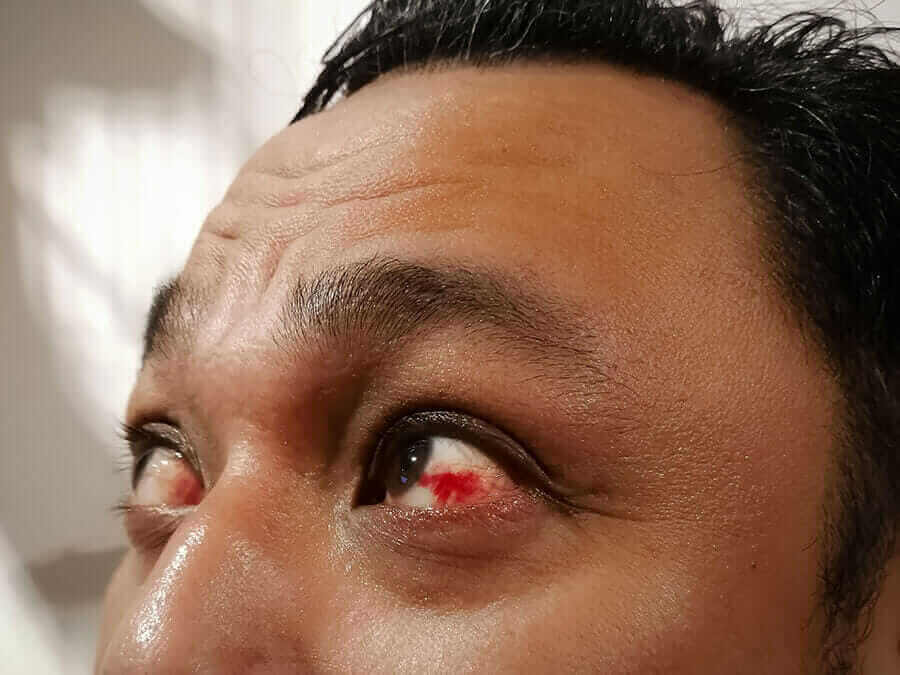
Eye trauma: If you have sustained an eye injury, such as a foreign object embedded in the eye or a chemical exposure, seek immediate medical care.
Severe light sensitivity (photophobia): Experiencing extreme sensitivity to light, to the point where it is unbearable, may indicate a serious eye infection or condition.
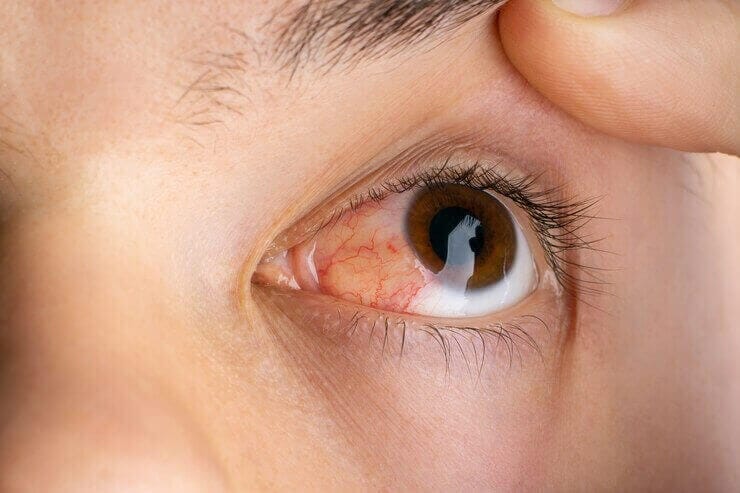
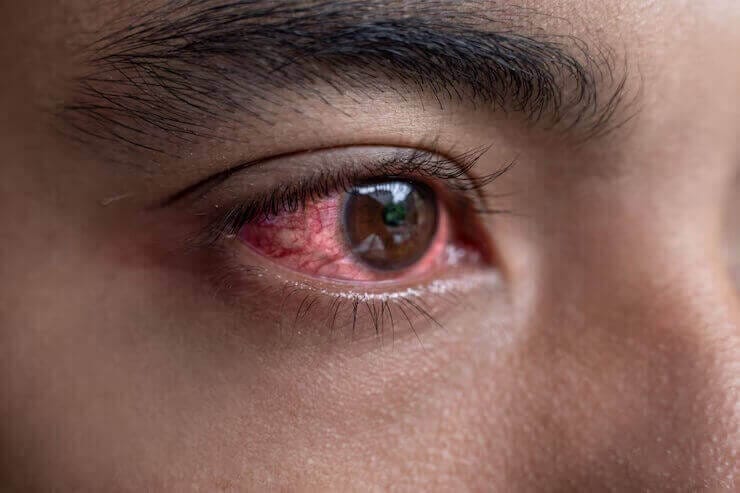
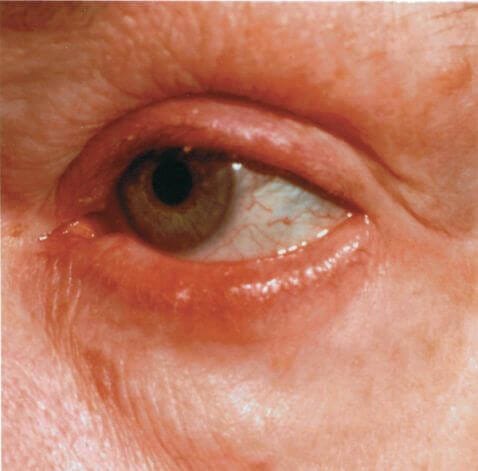
Severe Redness and swelling: If your eye is extremely red, swollen, and painful, it could be a sign of a severe infection or inflammation.
Blurred or distorted vision: Vision that becomes suddenly blurred or distorted, especially if accompanied by other symptoms, is cause for concern.
Discharge or pus: Thick, yellow or green discharge from the eye, is generally a sign of a bacterial, viral, allergic, or gonococcal conjunctivitis. However when these symptoms are accompanied by pain and redness, that may indicate an infection that requires immediate attention and should be seen by an optometrist.
Fever: If you have a fever in addition to eye symptoms, it could suggest a systemic infection that needs prompt medical evaluation.
Foreign body sensation: If you feel like there's something stuck in your eye, don't try to remove it yourself; instead, seek professional care. Learn more about foreign body sensation.
Double vision: Double vision that appears suddenly or is persistent should be investigated by a healthcare professional. Learn more about double vision.
Eye swelling with facial swelling: Swelling around the eyes, particularly if it spreads to the face, could be indicative of a serious infection or allergic reaction.
Eye pain with a history of recent eye surgery or injury: If you've recently had eye surgery or sustained an eye injury and experience severe pain with or without accompanying infection symptoms, contact an optometrist for an emergency eye exam.
Severe headache: A severe headache associated with eye pain, eye infections, or vision changes can indicate a potentially serious condition, such as glaucoma.
Loss of peripheral vision or tunnel vision: A sudden loss of peripheral vision can be a sign of conditions like retinal detachment or acute angle-closure glaucoma.
Eye symptoms in an infant or young child: If a child has eye redness, discharge, or other concerning symptoms, it's important to seek pediatric eye care promptly.
Infectious endophthalmitis is an emergency condition that requires urgent referral to an ophthalmologist and may be associated with cataract surgery, intravitreal injections, trauma, or systemic infections.